|
MOGAD, myelin oligodendrocyte glycoprotein antibody-associated disease AQP4-IgG+NMOSD, aquaporin-4-IgG seropositive neuromyelitis optica spectrum disorder MS, multiple sclerosis. Unilateral left optic nerve T2-hyperintensity on T2-weighted images (D 1, coronal view, arrow, and D 3, axial view, arrow), with a corresponding short segment of gadolinium-enhancement on T1-post-gadolinium images (D 2, coronal view, arrow, and D 4, axial view, arrow). Bilateral optic chiasm T2-hyperintensity on T2-weighted images (C 1, coronal view, arrows, and C 3, axial view, arrow) and optic chiasm enhancement on T1-post-gadolinium images (C 2 coronal views, arrow, and C 4, axial view, arrow). Unilateral left optic nerve T2-hyperintensity on T2-weighted images (B 1, coronal view, arrow, and B 3, axial view, arrow) and longitudinally extensive enhancement of the left optic nerve on T1-post-gadolinium images (B 2, coronal view, arrow, and B 4, axial view, arrow). Bilateral optic nerve sheath thickening (A 1, coronal view, arrows) and optic nerve T2-hyperintensity (A 3, axial view, arrows) on T2-weighted images, and corresponding longitudinally extensive optic nerve and sheath enhancement on T1-post gadolinium images (A 2, coronal view, arrows, and A 4, axial view, arrows). Orbital fat-saturated MRI in optic neuritis with MOGAD, AQP4-IgG+NMOSD, and MS. MOG NMOSD demyelinating diseases differential diagnosis false positive multiple sclerosis neuromyelitis optica.Ĭopyright © 2022 Sechi, Cacciaguerra, Chen, Mariotto, Fadda, Dinoto, Lopez-Chiriboga, Pittock and Flanagan. In summary, this article will review our rapidly evolving understanding of MOGAD diagnosis and management. 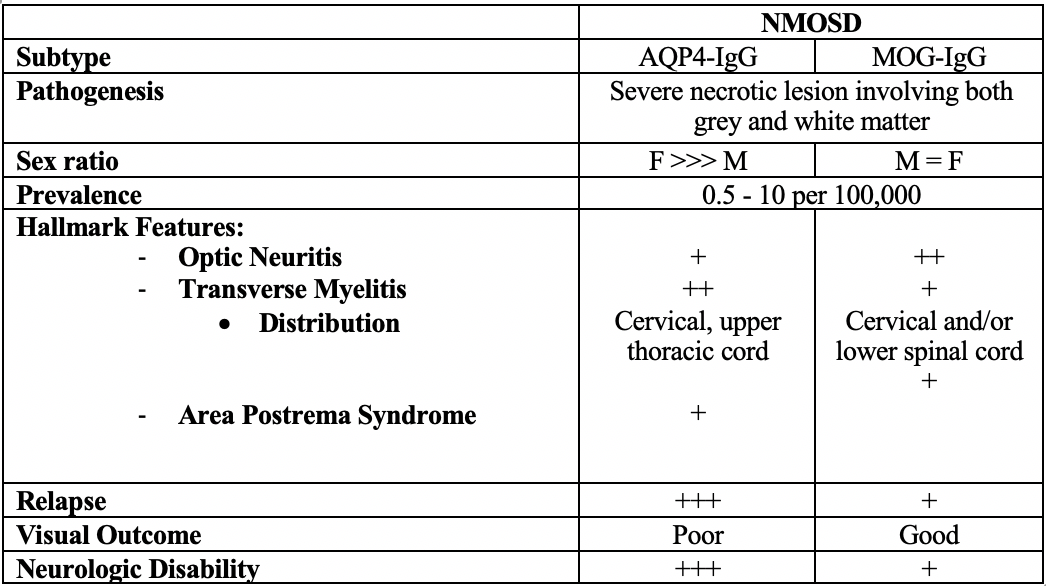
A variety of empiric steroid-sparing immunosuppressants can be considered and may be efficacious based on retrospective or prospective observational studies but prospective randomized placebo-controlled trials are needed to better guide treatment. Attack-prevention treatments also lack class-I data and empiric maintenance treatment is generally reserved for relapsing cases or patients with severe residual disability after the presenting attack. Although randomized controlled trials are lacking, MOGAD acute attacks appear to be very responsive to high dose steroids and plasma exchange may be considered in refractory cases. International consensus diagnostic criteria for MOGAD are currently being compiled and will assist in clinical diagnosis and be useful for enrolment in clinical trials. high) can influence the likelihood of MOGAD diagnosis. The type of cell-based assay used to evaluate for MOG-IgG (fixed vs. The detection of MOG-IgG in the serum (and sometimes CSF) confirms the diagnosis in patients with compatible clinical-MRI phenotypes, but false positive results are occasionally encountered, especially with indiscriminate testing of large unselected populations. Characteristic MRI features have been described that increase the diagnostic suspicion (e.g., perineural optic nerve enhancement, spinal cord H-sign, T2-lesion resolution over time) and help discriminate from MS and AQP4+NMOSD, despite some overlap. A relapsing course is observed in approximately 50% of patients. The clinical manifestations of MOGAD are heterogeneous, ranging from isolated optic neuritis or myelitis to multifocal CNS demyelination often in the form of acute disseminated encephalomyelitis (ADEM), or cortical encephalitis. 
Over the last decade, several studies have helped delineate the characteristic clinical-MRI phenotypes of the disease, allowing distinction from aquaporin-4 (AQP4)-IgG-positive neuromyelitis optica spectrum disorder (AQP4-IgG+NMOSD) and multiple sclerosis (MS). Myelin oligodendrocyte glycoprotein (MOG) antibody-associated disease (MOGAD) is the most recently defined inflammatory demyelinating disease of the central nervous system (CNS).
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
